COVID-19 Links
APC is providing the following information from the CDC and other resources regarding the Coronavirus and COVID-19. We are making these links available to provide you with the most current and relevant information.
APC is providing the following information from the CDC and other resources regarding the Coronavirus and COVID-19. We are making these links available to provide you with the most current and relevant information.

The outbreak of coronavirus disease 2019 (COVID-19) may be stressful for people, and especially those older than 60. Fear and anxiety about a disease can be overwhelming and cause strong emotions in adults and children. Stress during an infectious disease outbreak can include:
Why some people are more stressed than others about COVID
How you respond to the outbreak can depend on your background, the things that make you different from other people, and the community you live in. People who may respond more strongly to the stress of a crisis include:
Information has been extracted from CDC, Stress and Coping

Since early reports revealed that a new coronavirus was spreading rapidly between people, researchers have been trying to pin down whether it can travel through the air. Health officials say the virus is transported only through droplets that are coughed or sneezed out — either directly, or on objects. But some scientists say there is preliminary evidence that airborne transmission — in which the disease spreads in the much smaller particles from exhaled air, known as aerosols — is occurring, and that precautions, such as increasing ventilation indoors, should be recommended to reduce the risk of infection.
In a scientific brief posted to its website on 27 March, the World Health Organization said that there is not sufficient evidence to suggest that SARS-CoV-2 is airborne, except in a handful of medical contexts, such as when intubating an infected patient.
But experts that work on airborne respiratory illnesses and aerosols say that gathering unequivocal evidence for airborne transmission could take years and cost lives. We shouldn’t “let perfect be the enemy of convincing”, says Michael Osterholm, an infectious-disease epidemiologist at the University of Minnesota in Minneapolis.
“In the mind of scientists working on this, there’s absolutely no doubt that the virus spreads in the air,” says aerosol scientist Lidia Morawska at the Queensland University of Technology in Brisbane, Australia. “This is a no-brainer.”
When public health officials say there isn’t sufficient evidence to say that SARS-CoV-2 is airborne, they specifically mean transported in virus-laden aerosols smaller than 5 micrometres in diameter. Compared with droplets, which are heftier and thought to travel only short distances after someone coughs or sneezes before falling to the floor or onto other surfaces, aerosols can linger in the air for longer and travel further.
Most transmission occurs at close range, says Ben Cowling, an epidemiologist at the University of Hong Kong. But the distinction between droplets and aerosols is unhelpful because “the particles that come out with virus can be a wide range of sizes. Very, very large ones right down to aerosols”, he says.
And if SARS-CoV-2 is transmitting in aerosols, it is possible that virus particles can build up over time in enclosed spaces or be transmitted over greater distances.
Aerosols are also more likely to be produced by talking and breathing, which might even constitute a bigger risk than sneezing and coughing, says virologist Julian Tang at the University of Leicester, UK. “When someone’s coughing, they turn away, and when they’re sneezing, they turn away,” he says. That’s not the case when we talk and breathe.
A study of people with influenza found that 39% of people exhaled infectious aerosols. As long as we are sharing an airspace with someone else, breathing in the air that they exhale, airborne transmission is possible, says Tang.
Evidence from preliminary studies and field reports that SARS-CoV-2 is spreading in aerosols is mixed. At the height of the coronavirus outbreak in Wuhan, China, virologist Ke Lan at Wuhan University collected samples of aerosols in and around hospitals treating people with COVID-19, as well as at the busy entrances of two department stores.
In an unreviewed preprint, Lan and his colleagues report finding viral RNA from SARS-CoV-2 in a number of locations, including the department stores.
The study doesn’t ascertain whether the aerosols collected were able to infect cells. But, in an e-mail to Nature, Lan says the work demonstrates that “during breathing or talking, SARS-CoV-2 aerosol transmission might occur and impact people both near and far from the source”. As a precaution, the general public should avoid crowds, he writes, and should also wear masks, “to reduce the risk of airborne virus exposure”.
Another study failed to find evidence of SARS-CoV-2 in air samples in isolation rooms at an outbreak centre dedicated to treating people with COVID-19 in Singapore. Surface samples from an air outlet fan did return a positive result, but two of the authors — Kalisvar Marimuthu and Oon Tek Ng at the National Centre for Infectious Diseases in Singapore — told Nature in an e-mail that the outlet was close enough to a person with COVID-19 that it could have been contaminated by respiratory droplets from a cough or sneeze.
A similar study by researchers in Nebraska found viral RNA in nearly two-thirds of air samples collected in isolation rooms in a hospital treating people with severe COVID-19 and in a quarantine facility housing those with mild infections. Surfaces in ventilation grates also tested positive. None of the air samples was infectious in cell culture, but the data suggest that “viral aerosol particles are produced by individuals that have the COVID-19 disease, even in the absence of cough”, the authors write.
The WHO writes in its latest scientific brief that the evidence of viral RNA “is not indicative of viable virus that could be transmissible”. The brief also points to its own analysis of more than 75,000 COVID-19 cases in China that did not report finding airborne transmission. But Ben Cowling says that “there wasn’t a lot of evidence put forward to support the assessment” and, an absence of evidence does not mean SARS-CoV-2 is not airborne. The WHO did not respond to Nature’s questions about the evidence in time for publication.
Scientists in the United States have shown in the laboratory that the virus can survive in an aerosol and remain infectious for at least 3 hours4. Although the conditions in the study were “highly artificial”, there is probably “a non-zero risk of longer-range spread through the air”, says co-author Jamie Lloyd-Smith, an infectious-diseases researcher at the University of California, Los Angeles.
Leo Poon, a virologist at the University of Hong Kong, doesn’t think there’s enough evidence yet to say SARS-CoV-2 is airborne. He’d like to see experiments showing that the virus is infectious in droplets of different sizes.
Whether people with COVID-19 produce enough virus-laden aerosols to constitute a risk is also unknown, says Lloyd-Smith. Air sampling from people when they talk, breathe, cough and sneeze — and testing for viable virus in those samples — “would be another big part of the puzzle”, he says. One such study failed to detect viral RNA in air collected 10 centimetres in front of one person with COVID-19 who was breathing, speaking and coughing, but the authors didn’t rule out airborne transmission entirely.
Another crucial unknown is the infectious dose: the number of SARS-CoV-2 particles necessary to cause an infection, says Lloyd-Smith. “If you’re breathing aerosolized virus, we don’t know what the infectious dose is that gives a significant chance of being infected,” he says. An experiment to get at that number — deliberately exposing people and measuring the infection rate at different doses — would be unethical given the disease’s severity.
Whatever the infectious dose, length of exposure is probably an important factor too, says Tang. Each breath might not produce much virus, he says, but “if you’re standing beside [someone who’s infected], sharing the same airspace with them for 45 minutes, you’re going to inhale enough virus to cause infection”.
But capturing those small concentrations of aerosols that, given the right combination of airflow, humidity and temperature, might build to an infectious dose over time, is “extremely difficult”, says Morawska. “We could say that we need more data, but then we should acknowledge the difficulty of collecting the data,” she says.
The assumption should be that airborne transmission is possible unless experimental evidence rules it out, not the other way around, says Tang. That way people can take precautions to protect themselves, he says.
Increasing ventilation indoors and not recirculating air can go some way to ensuring that infectious aerosols are diluted and flushed out, says Morawska. Indoor meetings should be banned just in case, she says.
Meanwhile, Lan and others are calling for the public to wear masks to reduce transmission. Masks are ubiquitous in many countries in Asia. In the United States and some European countries, however, health officials have discouraged people from wearing them, in part because supplies are low and health-care workers need them. The Czech Republic and Slovakia, however, have made it mandatory for people to wear masks outside the home. Tang thinks those countries have taken the right approach. “They are following the southeast Asia approach. If everyone can mask, it is double, two-way protection,” he says.
But Cowling thinks masks should be recommended for the public only after supplies have been secured for health-care workers, people with symptoms, and vulnerable populations such as the elderly.

LONDON (AP) — Un-baaaaa-lievable: This wild bunch is completely ignoring rules on social distancing.
With humans sheltering indoors to escape the new coronavirus, mountain goats are taking advantage of the peace and space to roam in frisky clumps through the streets of Llandudno, a town in North Wales.
Andrew Stuart, a video producer for the Manchester Evening News, has been posting videos of the furry adventurers on his Twitter feed and they are racking up hundreds of thousands of views.
He said the goats normally keep largely to themselves, in a country park that butts up against Llandudno. But now emboldened by the lack of people and cars, the long-horned animals are venturing deeper into the seaside town. The U.K. has been in lockdown for the past week to combat the spread of the coronavirus.
“There’s no one around at the moment, because of the lockdown, so they take their chances and go as far as they can. And they are going further and further into the town,” Stuart told The Associated Press in an interview Tuesday from his parents’ pub in Llandudno, where he is waiting out the pandemic.
His videos show the goats munching on people’s neatly trimmed hedges and trees in front yards and loitering casually on empty streets as if they own the place.
“One of the videos on my Twitter shows that they were on a narrow side street and I was on the other side and they were scared of me. They were edging away from me. So they are still scared of people,” Stuart said. “But when there’s hardly anyone around on the big streets, they are taking their chances, they are absolutely going for it. And I think because it’s so quiet, and there’s hardly anyone around to scare them or anything, that they just don’t really care and are eating whatever they can.”
For most people, the new coronavirus causes mild or moderate symptoms, such as fever and cough that clear up in two to three weeks. For some, especially older adults and people with existing health problems, it can cause more severe illness, including pneumonia, and death.
Source: https://www.yahoo.com/news/un-baaaaa-lievable-goats-invade-152428950.html

In Wuhan China there have been a handful of cases reported including healthcare workers and a physician who tested positive, were sick and then had a negative test only to later be tested again and have a positive test. It has not been determined whether testing was faulty or this represents reinfection. Most infectious disease experts feel that reinfection is not possible. Ref: Lancet Viral dynamics in mild and severe cases of COVID-19, March 19, 2020 (20) 30232-2
After the quarantine/isolation/stay-at-home orders stop, will the disease stop spreading?

Absolutely not. There will be second waves of the disease even in countries that have effectively suppressed the first round. Two of these countries are Taiwan and Singapore who have experienced previous outbreaks from China, including SARS. They effectively quarantined sick people, isolated and ordered stay-at-home. They shuttered their economies used tracing methods and systematic tracking techniques. These have worked effectively but the virus is still in the general population particularly in asymptomatic infected people. They will spread the disease and symptomatic cases will occur again. This is going to happen in America. There will be a more severe round in multiple waves of the disease as we have not followed the same rigid even contact tracing, tracking, rigid isolation, extensive testing of symptomatic and asymptomatic patients along with other draconian measures. There will be waves of this as the virus runs its course. Two factors that will affect this are herd immunity and the development of the vaccine.
It is interesting to note that the Spanish flu 1918 was noted to still be in circulation and an active source of infection albeit in relatively low numbers through 2009 when the new version of H1N1 arrived.
There will be reservoirs of the virus in third world nations and densely populated areas. While the first world may be able to help mitigate and control this unless the Middle East, sub-Sahara Africa, Malaysia, Indonesia and India can control this virus will continue to re-infect the rest of the world until a vaccine. If the virus can hang around long enough it can mutate. We have experience with this. This occurred with the Spanish flu when a new strain developed a year after the original strain in 1919 and re-infecting the world.

In various opinions by epidemiology experts the real number of infections is likely 7-8 times as large. In a way this is good news, the disease is not as devastating or deadly as the numbers show. In other words, for eight people who get the infection, seven of them have sub-clinical or mild symptoms and may not be aware that they are sick and only one of these people shows overt disease. At Oxford, a theoretical epidemiologist has questioned the “Imperial model” of this virus. If this is correct and data from multiple sources support it is likely that the infection is substantially greater number than reported by the actual numbers of COVID-19 cases. This means that there are huge numbers of silent asymptomatic infected carriers. They are the silent carriers of the disease that can transmit this to the susceptible population, the aged and those with chronic illnesses. Social distancing, isolation, stay-at-home work and appropriate precautions can help minimize the immediate spread of this disease flattening the curve of transmission. This will minimize acute spread of the disease while immunity builds up in the population.
Bottom line: Everyone must act as if they are part of the large silent asymptomatic infected carriers or are interacting with a silent asymptomatic infected carrier when dealing with matters of personal distance, handwashing and social isolation. Think about your risk to friends, family and particularly the elderly and infirm in your life.
NO, ABSOLUTELY NOT!
I know of patients who are unable to be tested yet clearly had symptoms consistent with moderate infection. Since they were not sick enough to be admitted to the hospital, IDPH, Illinois Department of Health does not test. Estimates on asymptomatic, covert disease range from 31 to 60%.
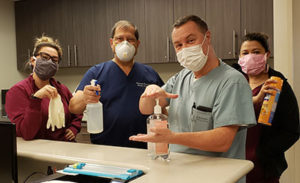
APC Bottom line: Everybody around you is a potential source of COVID–19. We worry about being around those who are sick or show signs of illness. The reality is three quarters of people who have the COVID–19 disease do not show any symptoms. Treat everybody as a potential infectious source. Practice social distancing. Continue with handwashing and hand alcohol. Continue disinfecting surfaces.
America is grossly ill-prepared to test adequate numbers of people. Currently Germany has the capability of performing 300,000 COVID–19 tests in a week. In America we have performed less than 600,000 total tests. The number of Covid-19 cases is grossly underestimated.
Among the most complete sites for information about spread of the Coronavirus (COVID -19) is the John Hopkins website. There is a map tracking COVID-19 cases around the world and it is excellent. See it at: https://coronavirus.jhu.edu/map.html
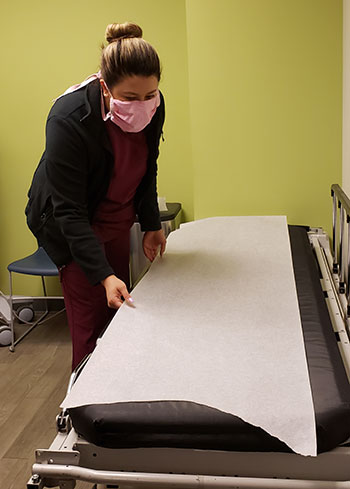
Our office is open and we continue to care for patients while adhering to the guidelines from the CDC, IDPH and other authorities regarding COVID–19 in this fluid and ever-changing environment. Our office, like all other medical practices, is considered an essential operation, and we will continue to make sure our patients pain management needs are a priority.
 What we are doing to help you:
What we are doing to help you:
We will always:
Interventional pain procedures, performed in our office, will be determined on a case by case basis to address the pain control needs of each patient. Our physicians will work with each patient to assess the option of proceeding or delaying the procedure. Postponing treatment is suggested if:
Our policies have been put in place to protect you, and those you come in close contact with, and our APC staff. Stay safe by protecting yourself, and monitor our website at apcnopain.com and our Facebook page, Advanced Pain Consultants for updates on COVID-19.
 At Advanced Pain Consultants, your health and safety are our top priorities. As your healthcare partner, we understand the concern you may feel about COVID-19.
At Advanced Pain Consultants, your health and safety are our top priorities. As your healthcare partner, we understand the concern you may feel about COVID-19.
We are carefully following all Centers for Disease Control and Prevention (CDC) and Illinois Department of Public Health (IDPH) recommendations and guidelines to ensure your safety in our facilities.
Preventing the spread of COVID-19 requires a global effort, and we all have a role to play.
Here’s what Advanced Pain Consultants is doing to keep you — and our greater community — safe:
What you can do:
You can help prevent the spread of COVID-19 by adhering to the following:
What should you do if you suspect you have COVID-19?
If you traveled recently to a known COVID-19 hotspot or have been in close contact with a confirmed COVID-19 patient and are experiencing symptoms, please contact your primary care physician for further guidance. There are specific recommendations for care based on your symptoms.
Additional resources:
The COVID-19 pandemic is a rapidly evolving situation. At Advanced Pain Consultants, we are closely monitoring these developments and will continue to offer guidance.
In the meantime, please access the latest information from the following organizations:
We’re here for you during this difficult time. Please contact us with any questions or to schedule an appointment. Thank you for your trust and support.
 There is a lot of anxiety and confusion relating the current Covid-19 epidemic. At APC, we are following CDC guidelines for distancing, handwashing, healthcare personal preventive equipment and thorough disinfection.
There is a lot of anxiety and confusion relating the current Covid-19 epidemic. At APC, we are following CDC guidelines for distancing, handwashing, healthcare personal preventive equipment and thorough disinfection.
The gold standard for information and guidance is the CDC and the WHO.
Containing and minimizing the viral outbreak is accomplished through isolation and minimizing contact. Patients and APC will operate on the following principles: